Graham Fraser Memorial Fellowship Report January 2004 to July 2004
Mr David K Selvadurai MD FRCS
Introduction
The Graham Fraser Memorial Fellowship is a combination of clinical training and research opportunities in otology. It offers unparalleled experience in cochlear implantation and the management of Meniere’s disease, constant constructive supervision from an international authority in otology and all this within one of the world’s most spectacular cities.
It was therefore an immense honour to be awarded the fellowship for 2004.
Preparation
The information provided by the foundation clearly explains the paperwork needed to obtain the Australian visa and medical license. Nonetheless the immigration related matters took many months to arrange, and alterations in health regulations lead to some last minute panics. Sue Alexander at the Royal Prince Alfred Hospital worked tirelessly at speeding things up with the registration process and I am sure I would not have made the start date without her help.
I was very fortunate in having a relative in Sydney with whom my family and I stayed until we were able to arrange our own flat. The favourable exchange rate with the UK allows you to rent a comfortable flat in a convenient location, and we chose to stay in the same area as the Mater Private Hospital where much of the operative work is undertaken.
The Fellowship
Professor Gibson is the Professor of Otolaryngology at the University of Sydney and Director of the Sydney Cochlear Implant Centre (SCIC). As such his work involves sessions at the Royal Prince Alfred Hospital, Westmead Children’s Hospital, The SCIC, The Mater Private Hospital and his own private rooms.
Unlike many other fellowships The Graham Fraser Memorial Fellowship allows the fellow to operate in both public and private sectors. This uniquely provides contrasts in service provision and greatly increases the amount of clinical material available. In fact the fellow undoubtedly gains more experience than an Australian trainee during the same time.
Professor Gibson operates on a two week time table covering the hospitals mentioned. Working at different locations does entail some travelling (usually with Prof) but each venue offers different clinical opportunities, work pressures and provides exposure to different teams.
The Royal Prince Alfred Hospital
The Royal Prince Alfred Hospital is the main teaching hospital for Sydney University Medical School and is Professor Gibson’s academic base. It is situated in cosmopolitan Newtown. As a teaching hospital it contains all the facilities you would expect such as a convenient library and IT resources which are available for use by the fellow. My main weekly activities here were observing otological surgery and neuro-otology with the registrars and attending various teaching events. The hospital provides a good location for meeting other surgeons, and I was able to observe Dr Pohl and meet Dr Halmagi here.
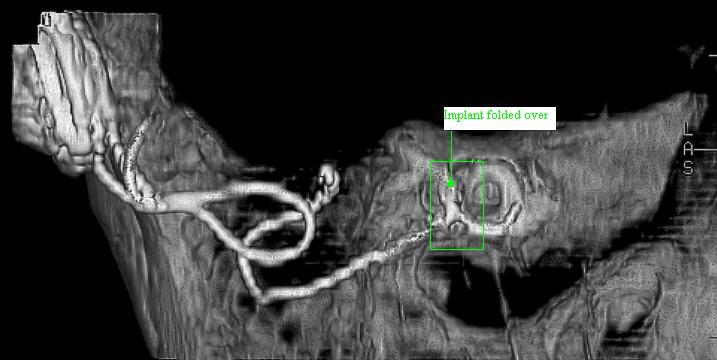
The department of radiology has recently acquired a CT system capable of reconstructing the structure of the middle ear in 3-D. This proved most useful in assessing a case of implant malplacement (see fig 1). I hope that I will be able to obtain such images in my unit in the UK in due course.
Figure 1 – “Folded over” implant demonstrated by 3-D CT
Professor Gibson’s Private Rooms
Prof has recently acquired a suite opposite the RPAH in Newtown. Within the suite there is a consulting room, a procedure room and audiology room with a sound proof booth. Prof conducts clinics at least four times per week. As the fellow I sat in with Prof and gained valuable insights into the assessment of the complex otology patient. Prof trained me to undertake transtympanic ECOG recordings in the procedure room. This is a useful skill to learn, and I took over this duty during the majority of the clinics. I also learnt how to perform transtympanic promontory stimulation and performed many such tests during the fellowship. I am now trying to develop a facility for transtympanic ECOG testing at my NHS unit.
Prof has built up a very large Meniere’s practice which allowed me to gain experience in the management of difficult scenarios such as bilateral disease and the treatment of resistance cases. For instance I became confident in the use of transtympanic gentamicin for vertigo control. By having a large cohort of Meniere’s patients it is also possible to follow the long term course of disease. This experience as made me very conservative in the use of destructive techniques, as it is clear that many patients develop bilateral disease as they grow older.
The promontory stimulation test has fallen out of favour in many UK units, and I rarely performed it in Nottingham. In Sydney all adult patients receive the test as part of their initial work up for candidacy evaluation. I soon realised the usefulness of the test. Many adult patients have not heard anything for some years and the sense of wonder they feel when they hear a crude electrical sound is amazing. I am sure that this experience motivates them and their relatives through the following months as they progress through assessment, surgery and mapping. It also provides great assistance in determining the side to implant.
The rooms are run by Cathy and Rosemary under the supervision of Alex Gibson. Together they provide a vibrant working environment and they are also a very useful source of local knowledge. By the end of the fellowship I felt a valued and integral part of the team.
The Princess Alexandra Children’s Hospital at Westmead
This hospital is situated in the western suburbs of Sydney. It is a new hospital which provides the most comprehensive paediatric service in New South Wales. It has been beautifully designed with the needs of children and their parents paramount. As such it was a pleasure and privilege to be on the staff here.
Prof uses this hospital for electrophysiological testing of children and also for cochlear implantation. The high levels of care available allow surgery on the very young, those with multiple medical problems and those needing multi disciplinary care. There are resident ENT registrars, but the fellow’s operating lists do not clash with the residents.
My weekly role at Westmead was to perform round window electrode placements under general anaesthetic for electrophysiological assessment of cochlear function. This involved surgery on babies down to a few months of age, which gave me great confidence in dealing with the middle ear in such infants. I had not previously performed such surgery on young babies. It is also a great opportunity to talk to Prof and Dr Sanli (the SCIC Biomedical Engineer) about the recordings and the problems of hearing assessment in the very young. Dr Sanli has firmly held views on the best testing methodology, and I became adept at reading the ECOG traces.
A unique feature of this testing regime is the ability to perform electrically stimulated auditory brainstem readings (EABR). This technique relies on a modified cochlear implant being used to feed a test signal through the round window electrode to stimulate an EABR. It is useful in the profoundly deaf ear where no ECOG threshold was detected. A clear response enabled the implant team to be very reassuring to the parents when discussing the likely outcome of implantation. Conversely a poor result, especially in conjunction with a poor radiological appearance to the Auditory nerve led to a very guarded prognosis.
I felt that for the parents of deaf children, who have many concerns and uncertainties, the information obtained from this rigorous assessment provided confidence in both the technology of modern cochlear implantation and in the team that was looking after their child.
Fortnightly Prof has a half day operating list at Westmead. Generally this is used for a cochlear implant (CI). The list provides excellent supervised operating with the fellow performing every case. Here I was able to progress from performing the cortical mastoidectomy at the beginning of the fellowship to being able to perform the whole implant procedure (without operative assistance, though supervised) at the end of my time.
I came across many unusual cases and in particular I will not forget a patient who had a bifid facial nerve, with one limb passing over the stapes. This case alone convinced me that continual facial nerve monitoring during cochlear implantation is necessary. Other interesting cases included CSF gushers and Mondini deformity cochleae.
The Sydney Cochlear Implant Centre (SCIC)
Every Wednesday I accompanied Prof to his clinic and CI meeting at this centre. The centre itself is housed in spacious accommodation in the grounds of the old Gladesville Psychiatric Hospital. As is often the case with such institutions the grounds are beautiful and provide a very pleasant working environment.
The weekly CI meetings are very educational. Issues relating to implantation problems in the SCIC population are discussed. As the centre has almost 1000 patients there are all manner of unusual problems to solve. The presence of experts in surgery, habilitation, speech therapy and electronics (namely Dr Sanli) allows for interesting discussions.
An interesting aspect of work here was the constant search for charitable funding. The programme has many streams of revenue but every opportunity to secure funding for one extra implant is used. This attitude had enabled the program to become the largest in Australia and is quite inspiring.
Many of the people at the centre have personal knowledge of the wonderful results of cochlear implantation as their children or partners are patients here as well. The whole environment was familial and the fellow is valued.
After the meeting I assisted Prof in the paediatric clinic, which is largely for seeing children referred for candidacy assessment. Prof implanted the world’s first paediatric multi channel CI recipient in 1987 and her amazing progress catalysed the development of CI programs across the world. Consequently the centre has an international reputation and receives many candidates from abroad. One such case proved to be the most challenging of my fellowship time.
Miss X was a fourteen year old child who had become deaf following meningitis one year previously. She had received a CI in her home country within a few weeks of the meningitis but had not been able to hear anything through it since it was implanted. Dr Sanli tested the implant and felt that it was working but that an alternative device type might be better. CT scanning showed that the other cochlear was ossified.
Prof and I operated on her a few weeks later. In a mammoth eight hour procedure we first repositioned and then replaced the first device, ultimately performing a cochlear drill out and laying a straight electrode array into the cochlea bed. Sadly intra-operative testing did not yield promising results and as planned we proceeded to the other ear. Here the cochlea was ossified, and on this side Prof inserted a double array.
I was pleased to hear that after considerable mapping and adjustment the patient is now receiving some useful audition, albeit less than we had first hoped for.
The Mater Hospital, North Sydney
Professor Gibson has all day operating at this private facility every other Friday and on other days as required. These days provide excellent surgical training. We often performed 3 CI and 2 other major ear cases in one list. Dr Sanli is present for most lists and his input is invaluable.
During CI operations Dr Sanli tests the implant before insertion, and then again after insertion. Using an implant derived EABR he can confidently tell the surgeon that the implant is correctly located and working. This information is relayed to the parents and carers on the ward and provides great reassurance some time before the patient is ready to return to the ward. Dr Sanli also provides intra-operative testing during stapedectomy, allowing the surgeon to be confident that a good result has been obtained.
Much of my surgical teaching was during the Mater lists. Profs teaching technique allows the fellow to progress according to his skill level. I never felt under-supported but always felt that I had made technical progress at the end of the week. This constant drive to improve helped me in many different areas. One example was my techniques for the Bone Anchored Hearing Aid (BAHA). I had performed this kind of surgery before but I learnt new ways around the common problems of excess bleeding and poor wound healing that often accompanies such operations. I felt that Prof’s teaching provided me with the best possible surgical “finishing school”.
The Mater hospital itself is luxurious and having been used to the décor and catering of the NHS working in a first class private hospital also provided a welcome insight into how pleasant the patient’s experience can be, when funding is more plentiful.
Educational Opportunities
In addition to the clinical teaching already outlined I was able to benefit from several special opportunities. The Australian Society of Head and Neck Surgeons (ASOHNS) annual meeting was in Sydney this year and I was able to attend this. Professor Gibson kindly funds the registration fees for the fellow. The conference covered many aspects of otolaryngology and gave me the opportunity to meet many interesting people. Amongst these were Professor Alec Salt from St Louis, USA, who is an expert in the field of cochlear micromechanics and perilymph flow. I was later able to hear him speak again at the New South Wales Meniere’s Society meeting and found his theories on the pathophysiology of this enigmatic condition fascinating.
I was also introduced to Professor Stephen O‘Leary from Melbourne. This proved to be a fruitful meeting as I was able to spend some time with him at the RPAH temporal bone dissection course, which I attended and assisted at. Dr O’Leary was able to show me the Virtual temporal Bone which he has been developing with the Commonwealth Scientific and Industrial Research Organisation (CSIRO), and which may well prove a useful adjunct to temporal bone dissection training for the future. The temporal bone course had excellent speakers from around Sydney, and I learnt a great deal.
I later visited Dr O’Leary and his colleagues in Melbourne. He kindly showed me around the hospital, laboratories and the Cochlear Companies facilities there. I was able to spend an afternoon with Dr Robert Briggs in the CI clinic and see a different approach to assessment of CI candidates. During my second day in Melbourne I spent time in theatre with Dr Briggs and Dr O’Leary. This was most useful as Dr Briggs is focusing his practice on hearing preservation during implantation, and showed me some of the surgical techniques that might enable this. The highlight of this trip though, was meeting Professor Graeme Clark at the Bionic Ear Institute. This was a great honour for me.
I also attended a satellite workshop at ASOHNS on facial-plastic surgery and was invited to Cochlear’s “Breaking the Silence” symposium on cochlear implantation in older age. This was a star studded event in the Natural History Museum. One of the most interesting speeches was from former Prime Minister Fraser. He recounted how, as minister for industry, he received a plea for extra funding from Professor Clarke to fund a little known technology called the multi-channel cochlear implant. He was sufficiently impressed by Professor Clarke’s commitment that he “took a chance” and supplied the necessary governmental support to complete the initial development and start the CI program. The rest, as he said “is history”.
Like some of the previous fellows I was also able to spend a day with the Royal Australian flying Doctors. Dr Neil Boustread, an ENT surgeon in North Sydney, and former fellow of Prof’s, flies out to Brewarina once every couple of months. I was able to join him and a registrar on this three hour plane flight into the outback. Medicine here is very different to downtown Sydney. The clinic building is well equipped but hospital facilities are distant. For instance a CT scan is a 2 day trip for the patient and is not untaken lightly!
One of the most bizarre things that happened during the fellowship was that during this flying doctors trip I met an old friend of my family’s from Sri Lanka. Dr Victor Benjamin has been a general practitioner in the outback for almost 20 years. He was Professor of General Surgery in Jaffna, Sri Lanka, but left during the civil unrest. He referred the second patient I saw that day and since I recognised his name I phoned and spoke to him. Three hours later, as we were finishing the clinic, Dr Benjamin and his wife appeared, having driven their 4X4 across the mud to meet me. I had not seen him since he visited my parents in Birmingham some 25 years ago. My father was delighted that I should happen upon his old friend and it struck me how small the medical world can be.
I was also able to spend some time with the other famous Professor of Otolaryngology in Sydney, Paul Fagan. I observed his unique techniques for dealing with canal exostoses and also watched him skilfully deal with a difficult revision stapedectomy. He performed this under local anaesthetic, and although it relies on a compliant patient, does offer a level of reassurance during high risk surgery.
Research Projects
The fellowship offers many opportunities for performing research projects. During my time I pursued three projects, two of which have progressed well. The first project was to look at the outcome of cochlear implantation in cases were there was radiological evidence of a hypoplastic auditory nerve. Detailed analysis of eight cases was performed, and although the outcomes were much poorer than in children with normal anatomy, there was evidence of some benefit. This partly contradicts the often quoted view that a hypoplastic nerve is a contra-indication to implantation. This paper is in preparation for submission to Cochlear Implantation International.
The second project was to analyse the results of over 1500 ECOGs performed during the last 7 years on patients with suspected Meniere’s disease and compare these to controls. This data is being prepared for submission to Acta and shows the diagnostic accuracy of tone burst testing compared to the traditional click AP/SP ratio.
The third project involved trying to assess whether a posteriorly placed cochlea led to a difficult electrode insertion. Professor Gibson presented on “the backwards twisted cochlea” at the Czech Republic for the Symposium on Hearing Disorders in Early Childhood in Prague in May 2004, and cited me as a co-author. It is hoped that further work on this subject may allow a full paper to be written in the future.
Social Events
Prof and Alex Gibson are wonderful hosts. My family and I enjoyed several trips out on Prof’s boat and we met again at many evening functions. One highlight was the cochlear dinner during ASOHNS. This was held at Fort Dennison on Pinchgut Island, which is situated in the middle of the bay and has tremendous views of the Bridge and Opera house.
Sydney is a fabulous city for a young family and we enjoyed our time there more than I can describe. We were also able to travel, and saw the Great Barrier Reef and the Blue Mountains. We sampled wine in Hunter Valley and went whale watching off Fraser Island. Our memories and photos have now bored our families, but remain very dear to us.
Career Benefits
I hoped and expected that undertaking this fellowship would make me more attractive to future employers but this belief was confirmed early in the year. A consultants post, with a special interest in Otology at St Georges Hospital was advertised in February. I returned from Sydney for the interview for this post and I was successful in obtaining it. During the interview it was quite clear that my further training in otology was of great interest and I am sure that it helped me secure the post.
Summary
I hope I have expressed the tremendous admiration I have for this fellowship. The training experience is unique, the city and country breathtaking and Professor Gibson is inspiring in so many ways. I feel greatly privileged to have been one of the Graham Fraser Memorial Fellows and my family and I are very grateful for the opportunities the fellowship has afforded us.
